Precision oncology: Advancing cancer care through new theranostics approaches
Provided by UChicago Medicine
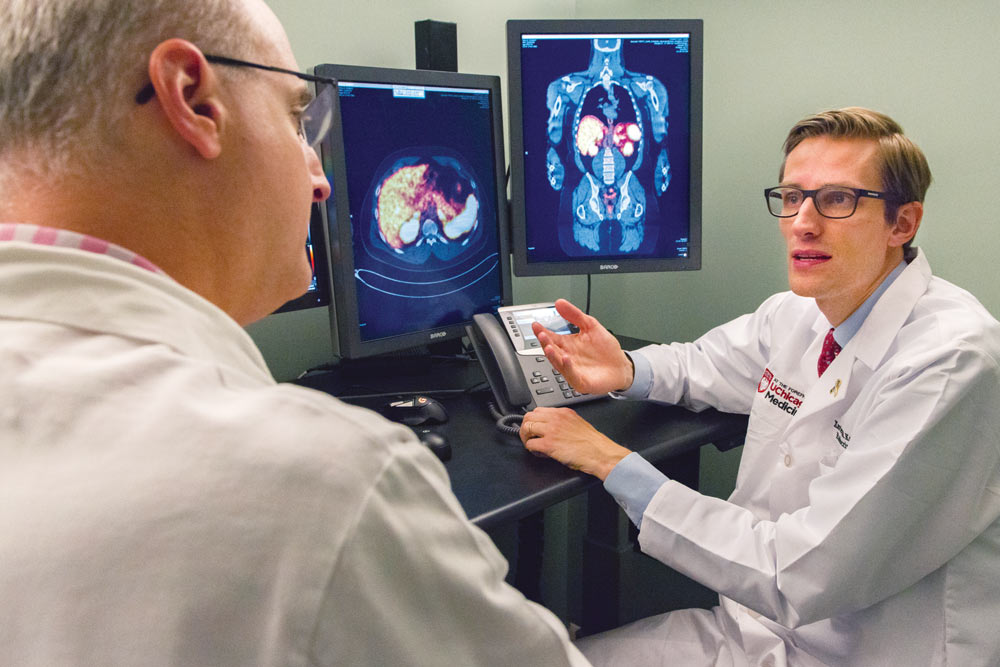
When Russell Szmulewitz, MD, describes an emerging tool used to diagnose and treat certain cancers, he can sound more like an Army general than an oncologist specializing in prostate cancer. Such is the precision of theranostics, however, that the analogy fits.
“It’s sort of a smart bomb that goes specifically to the cancer target, and we can see where it’s going based on the imaging piece,” said Russell Szmulewitz, Director of the Genitourinary Oncology Program at the University of Chicago Medicine.
Cancer theranostics – the word is a blend of “therapy” and “diagnostics” – involves the use of radioactive isotopes to diagnose and treat cancer. Physicians have been using radioactive isotopes like technetium-99 and strontium-89 to diagnose and treat cancer patients for years. Theranostics, however, uses radiotracers made up of two components: a biological component engineered to latch on to a specific protein on a cancer cell, and interchangeable radioactive isotopes that can alternatively make that cell visible on a PET scan and then kill it.
“Theranostics is sort of the ultimate in precision oncology because we can visualize the target within the patient, then give radioactive-targeted medicine that we know will go where we think we want it to,” Szmulewtiz said.
Diagnosis and treatment with theranostics do not occur all at once; patients first receive an IV infusion with the diagnostic radiotracer, then get one or a series of IV infusions with the radiotracer treatment a short time later.
“Then, a few months after your treatment, you might go back to get another scan with that diagnostic version of the tracer to see how the treatment worked,” said radiologist Daniel Appelbaum, MD, Chief of Nuclear Medicine and PET at UChicago Medicine.
The concept behind theranostics is not new. Radioactive iodine, for example, has been used for decades to both diagnose and treat thyroid cancer. (Rather than being guided to the cancer by a specific cancer cell-searching drug component, the iodine is absorbed naturally by the thyroid cells.)

New theranostics options offer new hope for our patients, helping them live longer and with better quality of life.
In recent years, physicians have been incorporating this more advanced iteration of theranostics to diagnose and treat certain neuroendocrine tumors (NETs), a rare type of cancer that begins in neuroendocrine cells, which are present in organs throughout the body. Xavier Keutgen, MD, Director of the Neuroendocrine Tumor Program, and Chih-Yi “Andy” Liao, MD, Associate Director of the Gastrointestinal Oncology Program, have been leading this effort.
“New theranostics options offer new hope for our patients, helping them live longer and with better quality of life,” Liao said.
Gallium-68 dotatate, copper-64 dotatate and lutetium-177 dotatate are all FDA-approved theranostic radiotracers that target somatostatin receptor 2, a protein that is over-expressed on the surface of NETs.
“From a diagnostic perspective, many studies have shown that gallium-68 dotatate or copper-64 dotatate PET-CT is vastly superior to any imaging modality for well-differentiated NETs,” said Xavier Keutgen, MD, an endocrine and neuroendocrine surgeon who directs the neuroendocrine tumor program. “When it comes to treatment with lutetium-177 dotatate, we’re talking about a benefit of several years in life expectancy for patients with NETs.”
Physicians are also hopeful about the use of theranostics for prostate cancer, a common cancer that affects one in eight men in their lifetime. UChicago Medicine was involved in the clinical trials for both piflufolastat F-18 and lutetium-177 PSMA-617. The FDA approved use of the former last year to diagnose certain prostate cancers and is expected to soon approve lutetium-177 PSMA-617 to treat metastatic, castration-resistant prostate cancer. Both of these radiotracers, along with diagnostic tracer gallium-68 PSMA-11, target prostate specific membrane antigen (PSMA), a protein on the surface of prostate cancer cells.
There are, of course, caveats with theranostics: Patients are exposed to radiation that may occasionally lead to developing other types of cancer, and the treatments are expensive and are typically not a cure. Cancer is clever, Appelbaum said, and the radiotracer doctors select to diagnose or treat a patient may not work on all of their cancer cells.
“You can have multiple metastases which behave differently in the same patient – they can have different genetic profiles,” said Appelbaum.
With the only academic health system cyclotron in Illinois capable of producing novel radioactive agents and in collaboration with Argonne National Laboratory, UChicago Medicine scientists are working to develop better theranostics that build off of those currently or soon available. Chin-Tu Chen, PhD, the scientific director of the UChicago Medicine Cyclotron Facility, is leading several studies, including one examining the effectiveness of using the same element, scandium, for both diagnosing and treating cancers.
“There are certain potential advantages to using scandium-43 and scandium-47 as a theranostic pair compared to gallium-68 and lutetium-177,” said Chen. “It’s the same element, so the pharmacokinetics will most likely be the same, and part of our research will be determining whether that’s clinically important or not.”
Chen is working with Szmulewitz, Keutgen and Appelbaum and a team of other experts to see if they can increase the number of cancer cell targets at which novel theranostics can take aim.
“We are still at the very early stages of theranostics, but we have the right people here, from basic scientists in chemistry working on new biomarkers, all the way to clinicians, and everybody’s within two blocks,” said Chen. “This is the model of team science.”
For more information, visit www.uchicagomedicine.org/global