A Framework for Achieving your Smart, Connected Hospital Vision
by Benjamin Kanter, MD, FCCP, Chief Medical Information Officer, Vocera

Hospital IT leaders have made massive investments over the last 20 years on digital technologies. They’ve built an electronic health record infrastructure. They’ve deployed digital technologies like wireless nurse call, digital radiology, and more.
And yet, too often, they’ve received too little value in return when these digital technologies are not connected and integrated within the clinical ecosystem.
To realize optimal value from digital data sources, a hospital needs to be “smart.” In other words, digital technologies need to be integrated within the clinical ecosystem through an intelligent clinical communication and collaboration (CC&C) platform.
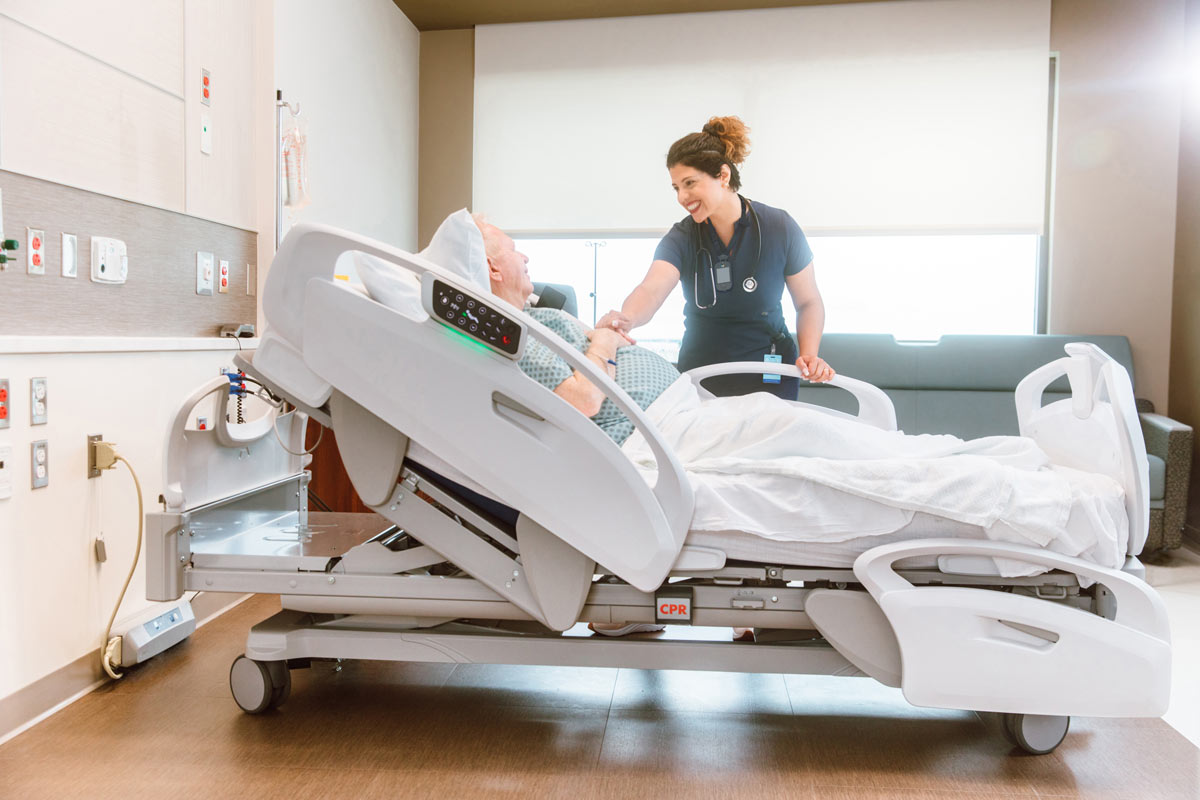
A smart hospital is one that leverages data from connected systems in near real-time. This is what enables nurses and physicians to rapidly derive insight and value from data sources so they can recognize and respond optimally to patient issues and provide better care.
In contrast, siloed technologies create workflow complexity for frontline care teams, who must focus more on dealing with the tools than on the work of patient care. Fragmented clinical communication and workflows have become untenable in the face of staffing shortages. And if the problem remains unchecked, complications will negatively affect patient safety and outcomes.
Smart, connected hospital framework
We developed a smart, connected hospital framework to help IT leaders visualize how to make the most of investments in their EHR infrastructure and clinical and operational systems – while improving the care team experience, patient safety and other outcomes. The framework illustrates how different types of interoperability work together in the clinical ecosystem starting with interconnected data sources and feeding upward into the end-user experience.
By connecting digital technologies within the clinical ecosystem and enabling deep interoperability, IT leaders can:
- Unify healthcare teams and the entire enterprise, tying together the clinical and administrative IT systems that are sources of data, information and knowledge.
- Align IT initiatives with a predetermined, well-constructed plan rather than managing clinical communication systems that grow organically without strategic governance or direction.
- Create a better work environment and experience for nurses, doctors and the extended care team – enabling a better experience for patients and families.
Deep interoperability and continuous process improvement
The smart, connected hospital framework consists of four layers which enable deep interoperability and continuous process improvement:
1. Input layer features data interoperability between clinical and operational systems such as the electronic health record, patient monitoring equipment, connected beds and medical devices. Data interoperability creates the foundation for connectedness.
2. Aggregation and intelligent processing layer includes intelligent middleware that enables routing, escalation and prioritization of clinical communications and alarm notifications at scale, delivered with associated context about the patient, event and care team.
3. Experience layer, where workflow interoperability enables people to receive information from multiple systems that has been aggregated and intelligently processed. End-user clinical communication devices reside at this layer and have bearing on how smart a hospital can be.
4. Analytics layer, where IT leaders measure clinical and economic outcomes and gauge the value they’re receiving from digital technology investments. For example, measure the average time to acceptance for bed exit alarms and set goals to drive down average response time. Continuous process improvement is a cornerstone in the development of a smart institution.
Download the ‘Smart, connect hospital framework’ whitepaper at www.vocera.com