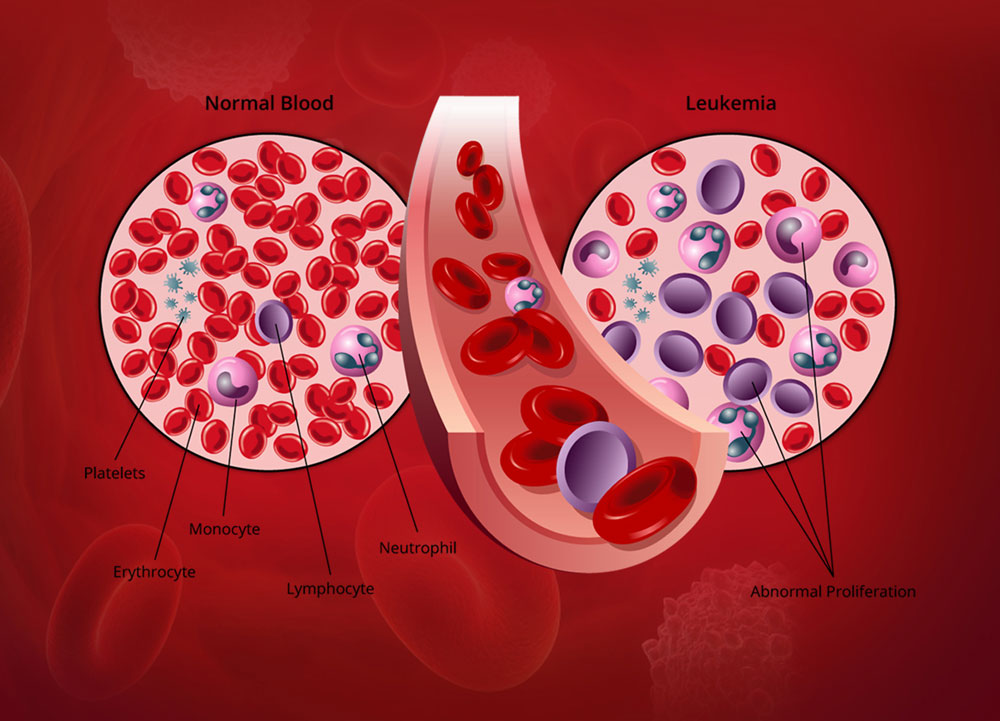
Leukemia
Uncontrolled growth of abnormal blood cells

Scientists haven’t found out yet the direct cause of cancer including leukemia; however, this did not discourage scientists from reaching effective and targeted treatments that increased the cure rate of some types of leukemia and control some other conditions contributing to the prolongation of patients’ lives.
The exact cause of leukemia is not known, but it is thought to involve a combination of genetic and environmental factors. Leukemia cells have acquired mutations in their DNA that cause them to grow abnormally and lose functions of typical white blood cells. It is not clear what causes these mutations to occur.
Causes of leukemia
Certain abnormalities cause the cell to grow and divide more rapidly and to continue living when normal cells would die. Over time, these abnormal cells can crowd out healthy blood cells in the bone marrow, leading to fewer healthy white blood cells, red blood cells and platelets, causing the signs and symptoms of leukemia. Over time, the leukemia cells crowd out or suppress the development of normal cells. The rate at which leukemia progresses and how the cells replace the normal blood and marrow cells are different with each type of leukemia.
In this context, we should explain that the blood contains 3 types of components including red blood cells, which carry oxygen, white blood cells, which fight infection and platelets, which help with blood clotting in addition to plasma, a liquid component of blood that normally holds the blood cells in whole blood in suspension and contains 90% of water.
Leukemia happens when the DNA of immature blood cells, mainly white cells, becomes damaged in some way. This causes the blood cells to grow and divide continuously, so that there are too many. Healthy blood cells die after a while and are replaced by new cells, which are produced in the bone marrow. The abnormal blood cells do not die when they should. They accumulate, occupying more space. As more cancer cells are produced, they stop the healthy white blood cells from growing and functioning normally, by crowding out space in the blood.
There are some risk factors that may increase your risk of developing some types of leukemia including:
- Previous cancer treatment: People who’ve had certain types of chemotherapy and radiation therapy for other cancers have an increased risk of developing certain types of leukemia.
- Genetic disorders: Genetic abnormalities seem to play a role in the development of leukemia. Certain genetic disorders, such as Down syndrome, are associated with an increased risk of leukemia.
- Exposure to certain chemicals: Exposure to certain chemicals, such as benzene — which is found in gasoline and is used by the chemical industry — is linked to an increased risk of some kinds of leukemia.
- Smoking: Smoking cigarettes increases the risk of acute myelogenous leukemia.
- Family history of leukemia: If members of your family have been diagnosed with leukemia, your risk of the disease may be increased.
Acute and chronic leukemia
Acute leukemia: During its lifespan, a white blood cell goes through several stages. In acute leukemia immature, useless cells develop rapidly and collect in the marrow and blood. They are squeezed out of the bone marrow too early and are not functional.
- The two most common types of acute leukemia are:
- Acute Lymphoblastic Leukemia (ALL)
- Acute Myeloid Leukemia (AML)
Chronic leukemia develops slowly and gradually, and symptoms may take a lot of time to develop. Sometimes chronic leukemia is diagnosed (through routine screening) before any symptoms develop. This is because the cancer cells in this condition are mature enough to perform their functions like normal white blood cells, before they begin to worsen.
There are two main types of chronic leukemia:
- Chronic Lymphocytic Leukemia (CLL)
- Chronic Myeloid Leukemia (CML)
Symptoms
Leukemia symptoms vary, depending on the type of leukemia. Common leukemia signs and symptoms include:
- Frequent fever or chills
- Persistent fatigue, weakness
- Frequent or severe infections
- Unexplained appetite loss or recent weight loss.
- Swollen lymph nodes, enlarged liver or spleen
- Easy bleeding or bruising
- Recurrent nosebleeds, bleeding from the gums or rectum, more frequent bruising, or very heavy menstrual bleeding.
- Tiny red spots in your skin (petechiae)
- Excessive sweating, especially at night
- Bone pain or tenderness
Evolution of treatments
There are a number of different medical approaches to the treatment of leukemia. Treatment will typically depend upon the type of leukemia, the patient’s age and health status, as well as whether or not the leukemia cells have spread to the cerebrospinal fluid. The genetic changes or specific characteristics of the leukemia cells as determined in the laboratory can also determine the type of treatment that may be most appropriate.
Treatments for leukemia include chemotherapy, radiation therapy, biological therapy, targeted therapy, and stem cell transplant. Combinations of these treatments may be used. Surgical removal of the spleen can be a part of treatment if the spleen is enlarged.
Acute leukemia needs to be treated when it is diagnosed, with the goal of inducing a remission (absence of leukemia cells in the body). After remission is achieved, therapy may be given to prevent a relapse of the leukemia. This is called consolidation or maintenance therapy. Acute leukemias can often be cured with treatment.
Treatment of most children with acute myeloid leukemia (AML) is divided into 2 main phases of chemotherapy: Induction and consolidation (intensification). In the induction phase, the chemo drugs most often used to treat AML are given for several days in a row. The treatment schedule may be repeated in 10 days or 2 weeks, depending on how intense doctors want the treatment to be. A shorter time between treatments can be more effective in killing leukemia cells, but it can also cause more severe side effects. Treatment with these drugs is repeated until the bone marrow shows no more leukemia cells. This usually occurs after 2 or 3 cycles of treatment.
Most children with AML will also get intrathecal chemotherapy (given directly into the cerebrospinal fluid, or CSF) to help prevent leukemia from relapsing in the brain or spinal cord. Radiation therapy to the brain is used less often.
In the consolidation (intensification) phase, about 85% to 90% of children with AML go into remission after induction therapy. This means no signs of leukemia are detected using standard lab tests, but it does not necessarily mean that the leukemia has been cured.
Consolidation (intensification) begins after the induction phase. The purpose is to kill any remaining leukemia cells by using more intensive treatment. Chronic leukemias are unlikely to be cured with treatment, but treatments are often able to control the cancer and manage symptoms. Some people with chronic leukemia may be candidates for stem cell transplantation, which does offer a chance for cure.