New Targeted and Individualized Method for Mechanically Ventilated Patients
Lateral positioning guided by electrical impedance tomography
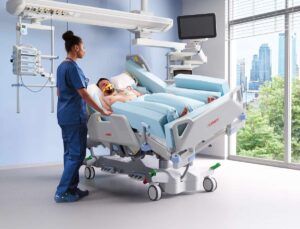
Can a hospital bed become a part of specialized therapeutic procedures and protocols? In case of highly sophisticated beds with integrated technology of controlled lateral tilt, the patient can without any effort be specifically positioned in order to optimize ventilation therapy.
This novel ventilation care is enabled by a combination of bed lateralization and continuous visualization of pulmonary ventilation continuous by means of non-invasive, radiation-free electrical impedance tomography (EIT) monitor. The method is based on advanced technologies from LINET and Timpel Medical.
Acceleration during the pandemic
Due to the COVID-19 pandemic, the care of mechanically ventilated patients has come to the forefront. In a cohorts of some of the larger epidemiologic studies of patients with COVID-19 to date, rates of invasive mechanical ventilation among patients admitted to ICUs range from almost 30% in one Chinese study (1) to 90% in a U.S. study (2) and elsewhere from 2.3% to 33.1% of patients admitted to the hospital. Invasive mechanical ventilation represents a cohort of patients with high morbidity and mortality rates that are associated with significant costs to the healthcare system.
The increase in numbers of patients and the severity of their health status required the deployment of all available means and procedures, but also accelerated the development and research of new technologies and approaches.
One of the innovative methods to optimize and individualize mechanical lung ventilation and effectively support the treatment of patients including those respiratory complications caused mainly by COVID-19 is a combination of controlled lateral positioning of the patient on the bed together with using electrical impedance tomography to monitor the effect. The spiritual father of this method is Michal Otahal, M.D., Ph.D. (General University Hospital, Prague Head of of Intensive Care Unit at the Department of Anaesthesia and Intensive Care). Another team of Prof. Marcelo Amato, M.D., Ph.D. (University of São Paulo, USP Department of Cardio-Pulmonary) is currently working on three clinical and experimental studies.

Individualized care for patients
The individualization of respiratory care using electrical impedance tomography and lateral body positioning provided by LINET and Timpel helps improve medical care in mechanically ventilated patients. Lateral tilting significantly influences the distribution of pleural and transpulmonary pressure and hence it allows physicians to manipulate ventilation distribution. However, this effect and its magnitude can vary signifficantly among the patients, thus robust monitoring tool of such effect is necessary.
Electrical Impedance Tomography (EIT) as a monitoring tool provides continuous real-time visualization of patients‘ ventilation. This is crucial in guiding ALT and ventilator settings. “By combining three devices, i.e. we can make sure that what we believed in really works. We can immediately change the strategy and adjust it to make it work better. We can quantify it, individualize it and it can be a little different for each patient. That is actually a bit of a problem of today’s medicine. We have general rules, but they do not work for everyone. Using a combination of these technologies, we can care for patients the way they need,“ explained Mikulas Mlcek, M.D., Ph.D. (Charles University in Prague – Experimental Physiology Lab Deputy-Director and the Head of Medical Simulation Centre).
In practice, this method works in such a way that the patient has a sensor strip attached around the chest, that captures data from which the EIT subsequently creates a dynamic ventilatory image of the lungs, not only globally, but importantly also regionally. Thus, the physician has immediate information about which lung regions are functionally affected and whether and which change in ventilator setting or body position is beneficial to the patient. The whole system can be imagined similarly to computed tomography, only the EIT, based on the change in the electrical impedance of the chest, displays a functional ventilation image of the lungs, non-invasively and without irradiation, which is a significant advantage over CT.
Technological shift
Scientific research dedicated to the concept is also reflected in the development of products that have enabled this breakthrough. “We came up with this concept around 2013. At that time, just the availability and use of the EIT was not at the level it is now,” confirmed Michal Otahal, M.D., Ph.D. LINET, meanwhile, has developed a new generation of the Multicare bed, which has expanded the existing options for lateral positioning. The programmed positioning cycle, automatic lateral therapy, can now be preset with up to four programs that make it easy to use ALT to tailor the patient’s indication. ALT can now also be combined with the anti-Trendelenburg position, making it possible to get the body into a more natural position. At the same time, the weight limit for patients was also increased. “We also know from experience that therapy can run for more than 24 hours. That’s why we’ve integrated Smart Pause Management, which allows you to discontinue therapy. The bed can then be freely positioned to facilitate the performance of necessary tasks, such as checking pressure ulcers. Subsequently, with the press of a button, you return to the last ALT position and the therapy can easily continue, ”describes LINET Product Manager Jan Michalek.

(1) Wang Y, Lu X, Chen H, Chen T, Su N, Huang F, et al. Clinical course and outcomes of 344 intensive care patients with COVID-19. Am J Respir Crit Care Med [online ahead of print] 8 Apr 2020; DOI: 10.1164/rccm.202003-0736L
(2) Richardson S, Hirsch JS, Narasimhan M, Crawford JM, McGinn T, Davidson KW, et al. Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York City area. JAMA 2020;323:2052–2059.