Prostate cancer became the most common malignancy in men and the second-leading cause of cancer death among male population. The only risks of developing prostate cancer (Pca) are being male gender and increased age. It has been much more commonly diagnosed after introduction of prostate specific antigen (PSA) test which led to widespread screening. PSA screening has been associated with increased diagnosis of Pca and a shift toward diagnosis of earlier-stage disease, concomitantly increasing surgical treatment and cure of the disease.
“Localized and/or locally advanced prostate cancer patients can safely be treated by radiation, minimally invasive methods, focal therapies and radical prostatectomy,” said Professor Rahmi Onur, Urologist specialized in Urinary Incontinence and Bladder Health, Diagnosis and Treatment of Prostate Diseases in Acıbadem Ataşehir Hospital, Istanbul.
Robotic radical prostatectomy utilizes the latest technology to treat PCa. It’s also been used in kidney, bladder and testicular cancer surgeries. In Acibadem Group, we have several Da-Vinci robotic systems and successfully perfom all robotic cases. This modality offers full robotic approach and there is no incision and no open surgery. Robotic radical prostatectomy is the gold standard treatment and a minimally invasive surgical treatment for organ-confined prostate cancer.
The “daVinci” Robotic System is a computer-based, minimally invasive robotic system, which consists of 3 main parts as surgical equipment that enables the operation to be performed with the least possible damage to the body. Robotic urological surgeries are not only confined to cancer treatment. Recently, renal transplantations are successfully completed by robotic Da-Vinci system. Other surgeries performed by robotic surgeries are simple prostatectomy, bladder stone diseases, ureteral and renal junction stenosis and pelvic organ prolapse.

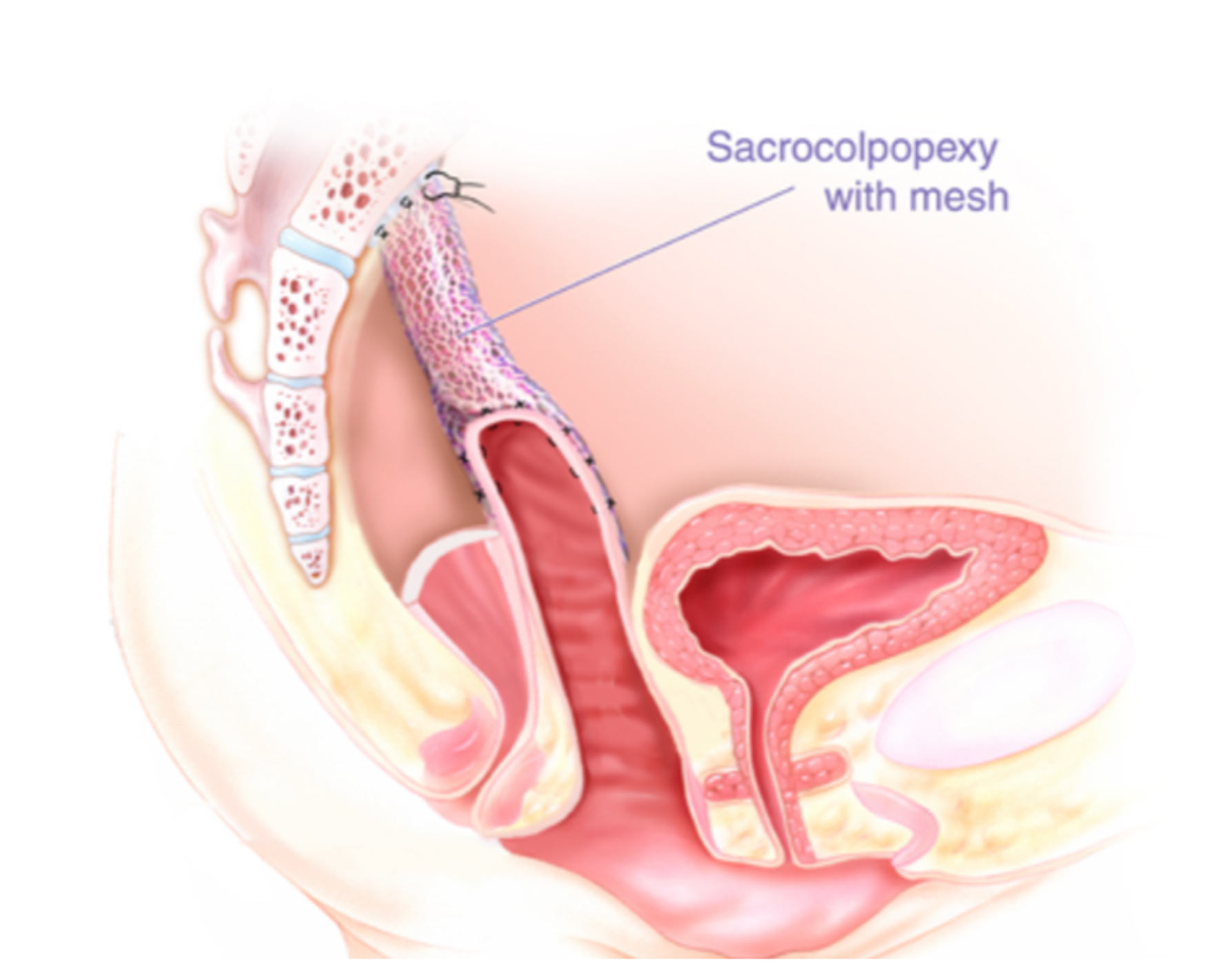
Pelvic organ prolapse is another urogynecology problem that occurs after multiple births, difficult births, interventional births, relaxation of the muscles that suspend the bladder (pelvic floor muscles). It commonly occurs after menopause or after removal of the uterus (hysterectomy) and some other gynecological surgeries. Mild prolapse cases can be treated by pelvic floor exercises or pessary use- however, severe uterine, vault or bladder prolapses bring severe symptoms and they need to be surgically treated. Thanks to the robotic technology, we can safely and successfully treat pelvic prolapses by robotic surgery too. In this method, uterine or vault prolapse is treated by robotic sacrocolpopexy or robotic hysteropexy. This involves mesh placement to the tip of vault and suturing this to the scral promontroium. It has more that 95% success rates in our hands. We perform the surgery as same-day or 1-day hospitalization surgery and use no drains or catheters. This has done totally through abdomen and with no incision.
Sacral Neuromodulation – Electrical Control of Urinary System
Lower urinary tract symptoms associated with voiding problems may arise from many different pathologies affecting pelvic organs, pelvic floor or both. Voiding dysfunction is a broad class of bladder conditions that ranges from urinary incontinence (inability to store urine) to urinary retention (inability to empty urine). There may be other bothersome symptoms, too.
Bladder problems are troublesome and decreases patient’s quality of life. Patient may leak small or large amounts of urine, or may not be able to empty her/his bladder completely. These problems can interfere with the individual’s lifestyle and make simple daily activities and social life difficult.
Symptoms
Most common symptoms of voiding dysfunction are:
- Urinary Urge Incontinence
- Urgency/Frequency
- Urinary Retention
- Fecal Incontinence
- Bladder pain/Pelvic pain
The problem
Voiding dysfunctions may be due to neurogenic problems bladder or idiopathic in origin. In the etiology, pelvic floor dysfunction and related events can cause an inappropriate “barrage” of signals that may cause a “miscommunication” between the pelvic floor and brain, resulting in these symptoms.
Management
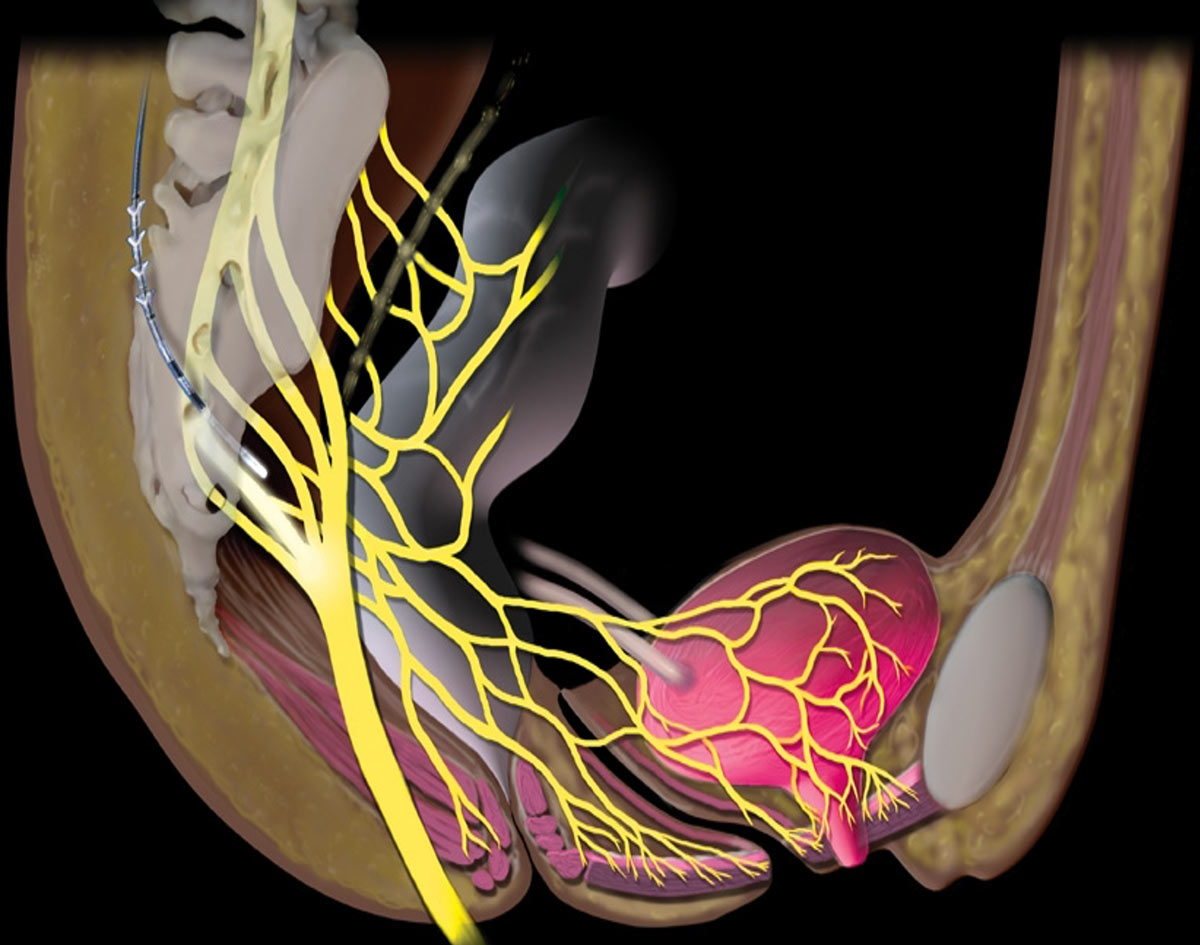
Sacral nerve root in the anterior surface of the bone is the key point for stimulation and for voiding physiology. Sacral nerves control:
- Bladder
- Bowel
- Urinary and Anal Sphincters
- Pelvic Floor Muscles
Sacral neuromodulation is a unique treatment modality with an implanted battery system that helps to coordinate: bladder, sphincter and pelvic floor. It also modulates reflex and neural activities.
This treatment electrically stimulates the sacral nerves that carry signals between the bladder and the brain. It is an implantable, MR safe and rechargeable system implanted in the sacral bone and upper buttock during a minimally invasive outpatient procedure.
With this externally programmable solution, patient can start, stop and adjust therapy.
Who are candidates for this treatment?
There are no contraindications for sacral stimulation. It’s commonly indicated in drug and behavioural treatment resistant OAB, idiopathic urinary retention, chronic pain, and fecal incontinence. Recently, it has been used in neurogenic bladder and spina bifida cases, too.