Streamlining for Safety: Barcode Medication Administration for Intravenous Medications
James Waterson. RN, M.Med.Ed. Medication Safety Manager, Medical Affairs. Becton Dickinson. Eastern Europe, Middle East and Africa.
James.waterson@bd.com
Radwa Elsawah. RPh. Product Manager. Medication Management Solutions. Becton Dickinson. Eastern Europe, Middle East and Africa.
Larry Neal. Regional Marketing Manager, Medication Management Solutions.Becton Dickinson. Eastern Europe, Middle East and Africa.

Potential errors of Wrong Patient, Wrong Medication, Wrong Dose, Wrong Documentation, and Wrong Time can all take place at the bedside, and among all the stages of the medication chain -from prescription to administration- medication errors which occur at the point of administration are the most prevalent at 68% of all IV medication errors. And with only a 2% chance of detection of error, in terms of Failure Mode Effect Analysis (FMEA) the IV administration process consistently scores as a high-risk activity by virtue of this difficulty of detection, with a Detectability Score of 10 (0 = Minimum Harm Risk – 10 = Maximum Harm Risk) commonly being applied by organizations utilizing FMEA.
This is the dangerous ‘gap’ that Connected Compounding Solutions and Interoperability Capable Infusion Pumps can close, as they effectively loop back IV medication administration directly to the original prescription and ensure completion of the documentation of administration. This can be achieved by bidirectional-interoperability capable IV pumps through direct communication with the patient’s Electronic Medical Record (EMR):
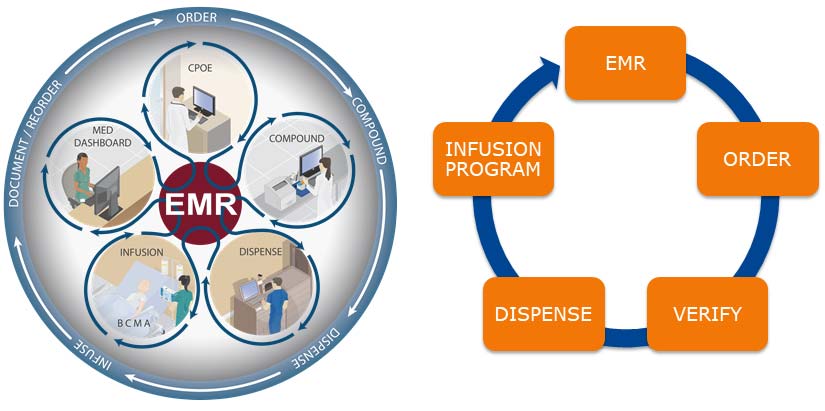
The barcode on the IV medication bag or syringe triggers this communication during a process of scanning the Patient’s ID band, scanning the medication to be given, and scanning the barcoded unique identifier of the IV pump. The pump is then triggered to communicate with the EMR and the confirmation with the Computerized Provider Ordering Entry system allows for auto-population of the pump with an order string that carries the correct dose, duration or rate, correct volume of the IV bag and the patient ID.
This is truly streamlined safety as it can also reduce the time spent programming the pump by over 80%, and healthcare needs streamlining badly. Up to 38% of a nurse’s time is spent on non-value added activities and these non-value costs can take millions of dollars per year out of an organization’s budget.
The hospital pharmacy is central to the above workflow as it is here where the order is electronically received from the CPOE, the medication is compounded and the individual and unique barcode with an order string is created from the CPOE, and the individual patient ID is created. It is possible to manage this process manually, but many of the critical steps involved in compounding carry potential error rates as high as 49%, and it is far better to have integration between the CPOE and the compounding software to avoid breaks in the medication chain, and to reduce the risk of transcription errors. Prescribing software should also include ‘Hard Stops’ for dosing and automation of calculations for Area Under the Curve (AUC) dosing. Ideally, the CPOE gives prescribers access to computer-based standardized protocols, which reduce non-standard regimen creation, can make for a faster regimen build, and automatically calculate doses and create preparation guidance. With integration, physician prescriptions can be received electronically into the pharmacy for verification, and if approved, for push-communication to the compounding unit.
Interoperability between the EMR and IV Pumps is an ideal solution for the whole hospital medication safety, as it requires an investment in communication engines to link pumps to the EMR and an organization-wide network capable of carrying these messages, ideally via secure wireless communication.
Modern smart pumps can make this a highly protected connection via Advanced Encryption Standard (AES) 128-bit key encryption using Cipher Block Chaining (CBC). This encryption applies to a vast number of connections with modern smart pump servers being able to manage up to 18,000 pump channels with full, and secure, bidirectional interoperability across hospital campuses with multiple sites.
As mentioned above, efficient compounding software is a central part of any EMR interoperability solution for IV medications, as every prescription must pass through the pharmacy for reconstitution and application of the unique patient-medication matched barcodes. The pharmacy compounding unit is truly the engine house of IV medication production and of IV medication safety. A compounding workflow software solution can undertake both preparation and documentation assistance and checks. A software suite should support initial pharmacist verification of the order, gravimetric checks, and incorporate a monitor inside the work area with a minimal interaction interface with step-by-step instructions. The software can propose a list of items that includes the minimum medication vials, diluents and consumables required to prepare the dose.
Scanning of individual components ensures a recipe match for all items including the final IV administration bag. The system must also carry ‘Hard Stops’ for dosing out of tolerance (usually ±4% tolerance is accepted by most institutions).
The compounding system should only deliver a patient-medication label after all the steps of compounding are successfully complete, which makes it ideal for building into an FMEA process, as the steps involving risk are all before the final verification checks and issuing of the label with a unique preparation and patient identification number.
The software must be capable of recording all cancelled mixes, tolerance limit breaches, incorrect item scans, and the resolutions of alerts by the user. Date-time stamps are automatically applied to all these alerts and actions by modern compounding solutions. This data is ideally stored locally on an MS-SQL database inside the hospital firewall. Documentation in the central pharmacy of compounding statistics for each preparation can be aggregated and this assists with forecasting.
Viewers and dashboards of the entire IV medication management process from prescription to administration help senior pharmacy managers to identify bottlenecks in the pharmacy fulfilment process. Compounding units can also view infusion status in all nursing units, allowing for just-in-time resupply of critical medications and prioritizing of activity and queuing of compounding requests. New medication dose requests are easily identifiable in such an arrangement, and such systems are extendable into inventory control and forecasting functions. Compounding software can also be used to extend medication safety beyond the pharmacy and into the nursing unit. This solution is a ‘lighter touch’ than full EMR bidirectional interoperability, though hybrid solutions with all the advantages of compounding software to smooth the workflow of production, married to barcode right patient-right medication verification via EMR-interoperability capable IV pumps, are also feasible. Medication safety should always be an ongoing journey to zero patient harm and scalability and adaptability of solutions, so called ‘futureproofing’ is a vital consideration for organizations when building their IV medication risk management strategies.
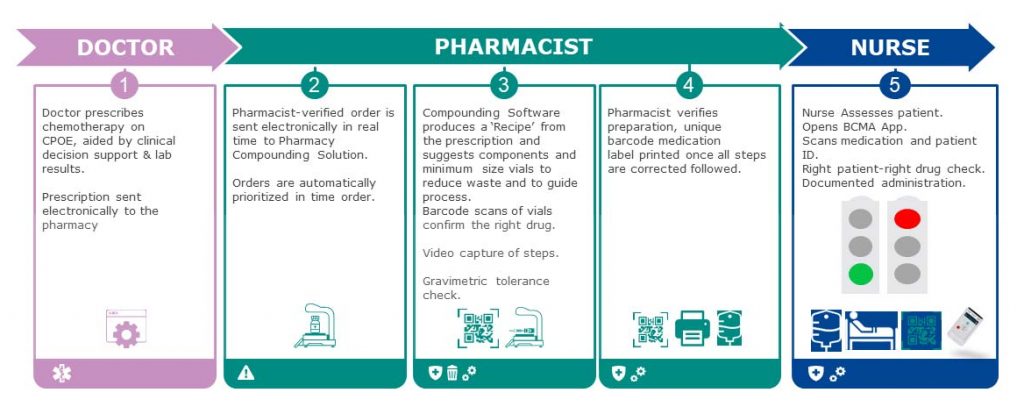
The ‘light touch’ solution requires less infrastructure and complexity as it can stand outside of the EMR or have touchpoint integration only, with access to Admission Discharge and Transfer (ADT) data from the EMR for example.
The below workflow shows how bedside BCMA scanning by nursing staff to support right patient-right medication verification at the bedside is supported by the compounding solution: (image on the right)
This requires the deployment of wireless connected handheld barcode scanners to the nursing unit. As the patient ID band and the patient-medication barcode label on each compounded product are scanned, this potential ‘match’ is transmitted to a ‘listening post’ interface and through to the compounding solution server, where the match is tested and if it is correct for patient, medication, dose, volume and regimen appropriateness (oncology regimens, of course, contain multiple medications and are timed and scheduled as per the CPOE order) the nurse gets a green light, and can proceed with administration.
This workflow achieves several things. It replaces a large amount of manual activity by nursing staff, and should reduce the risk of medication errors as it undertakes positive patient ID and matching of the compounded product to the patient. It also means this activity takes place directly at the bedside, avoiding the risk of checks being made at the nursing station and then a mix up occurring due to distraction or other error in the ‘last few metres’ to the patient. The two-nurse or ‘four-eyes’ check is also not required as the barcode acts to verify fully, and of course there are many reports of the ineffectiveness, dangers of positive reinforcement of error, and of time-wasting that occurs when verification is undertaken manually by two clinicians. Printed pages for regimens, which can be mislaid or placed in the wrong patient record, are also eliminated in this approach.
As discussed above, safety systems can also streamline practice. In a recent study in a high turnover oncology unit with 16,000 patient visits and over 14,000 compounded medications per annum the introduction of a compounding software solution with BCMA labelling saw a 35% reduction in the time required to compound each product.
The introduction of handheld barcode scanners for patient-medication verification led to patient verification time falling from ≈ 6 minutes to a mean average of only 41 seconds within two weeks of its introduction. When calculated against the checking of 14,000 medications this gives a saving of nursing time equivalent to 0.43 fulltime nurses per year. The savings for a 1,000-bed hospital compounding 40,000 oncology medications per year would be 1.21 full time nurses.
Technology cannot do everything that healthcare staff can do, but what it can do is release our most valuable asset, our highly skilled staff, to undertake patient work of real value and to allow them to work in an environment that supports them in keeping patients safe.