Sustainability & Healthcare: A Choice and an Urgent Necessity in Medication Management.
James Waterson. RN, M.MedEd, MHEc. Medical Affairs Manager, Medication Management Solutions. Becton Dickinson Middle East and Africa.
Aya Idriss. BSc. Product Specialist, Medication Management Solutions. Becton Dickinson Middle East, North Africa, and Turkey.
Tarek Kassab. MSc, MD. Market Access & Strategy Leader. Medication Management Solutions. Becton Dickinson Middle East, North Africa, and Turkey.

The Direct Challenge
One of the biggest challenges facing us today right across the healthcare continuum is sustainability. This means physically reducing the carbon footprint of healthcare, and reducing the consumption of plastics in the form of disposables and sterile packaging of medical supplies. This is undoubtedly important and at Becton Dickinson we strive to achieve these very clear goals through vigilant supplier oversight for adherence to applicable environmental laws and regulations. We also aim to optimize the environmental performance of products and operations and take a life-cycle approach for all products.
BD is committed to making strong efforts to reduce the consumption of energy, water, and other nonrenewable natural resources, as well as minimizing, measuring and reporting water and air discharges into the environment.1
The ‘Indirect’ Challenge.
At Becton Dickinson we view sustainability as a portfolio of complementary initiatives and actions that helps us achieve our purpose of Advancing the World of Health™. Our 2030+ sustainability strategy addresses a range of challenges in our industry while helping to make a difference on relevant issues that affect society and the planet.2
Of course, all of us working in healthcare have always had a responsibility to society and to our patients and to the individuals we work with in our healthcare facilities to deliver and sustain the highest quality of care right across the patient experience, from admission to discharge, and beyond. But now more than ever ecological and human sustainability needs to be built into every patient interaction. By putting sustainability front and centre in our approaches to patient care we can ‘build back’ into the system through managing care efficiently. Applying technology to care can help to reduce waste in terms of our human resources, facility resources in terms of Length of Stay (LOS), pharmaceutical and surgical treatment resources, and community resources.
BD works to strengthen healthcare systems across the world by developing and deploying market-appropriate solutions, and BD Global Public Health works to align activities, priorities, and development efforts around the world’s leading public health needs. We drive access to existing BD solutions and develop and deploy innovations to address priority health needs in areas aligned with Sustainable Development Goals (SDGs).3

Sustainability and Medication Management Solutions
Medication management has, as its core goal, avoiding iatrogenic harm. One example of this is planning for successful discharge, avoiding ‘bounce back’ readmission, and reducing the risk of self-medicating patients taking medications incorrectly, or not adhering to medication regimens due to lack of understanding. The question is how can we create this time for teaching and engaging with patients to take place in a busy outpatient pharmacy department?
A robotic and automated pharmacy may help us achieve the goal of protecting time for pharmacists to undertake techniques like ‘teach back’, and also review medication regimens for potential deprescribing and dangerous polypharmacy during discharge planning or outpatient education and help to ensure that patients adhere to medication regimens. A program of medication counselling and education may help reduce the ‘bouncing back’ we currently see, with one study showing that 14.7% of emergency admissions in Saudi Arabia were related to medications being taken incorrectly at home.4
Such events cost the system, cost social healthcare budgets, and cost the environment with the opportunity cost of dispensing never used, or incorrectly used, pharmaceuticals. To achieve this aim of pharmacists and nurses being able to spend more time on direct care and patient education we need to reduce the Non-Value Added (NVA) tasks that pharmacists and nurses undertake so that they can do the things they were trained to do. The 2016 study of Fisher et al suggested that pharmacists spend more than fifty percent of their time in traditional medication management systems in NVA tasks such as inventory, medication ordering, or undertaking double-checks on forecasts.5
We often think of waste in terms of discarded plastics and ‘simple’ extravagance or carelessness, but West’s Delphi panel of 2015 gave a stark warning on the impact of medication wastage and a very comprehensive description: ‘Medication wastage refers to any medication which expires or remains unused throughout the whole medicines supply chain. It also refers to the unnecessary or inappropriate consumption of medications by patients, or the unjustified non-adherence to treatment guidelines by healthcare professionals. Medication wastage poses a financial burden on patients themselves and the state’s economy and requires adequate education of all people concerned’.6 Medications are expensive for the organization and for society in simple monetary terms, but of course there is also an environmental cost and extensive use of ecological resources in the production of pharmaceuticals which can be wasted if the patient is non-adherent, if medications are given incorrectly, and of course if stock is not handled efficiently and pharmaceuticals expire in the facility.
Preservation of medication supply by reducing the risk of expiry can be substantially improved by the use of robotic pharmacies as the system takes in the expiry date along with other medication data via barcode reading and as it loads the secure storage area it looks for special precautions such as refrigeration requirements and arranges and rotates medications by expiry date and creates a dynamic inventory with alerts for slow moving items and near-expiry products. A 2022 outpatient study that assessed wastage via a ‘basket’ of sample medications, found expired medication wastage cost was reduced by 83.9% following the introduction of a BD Rowa™ robotic pharmacy for management and dispensing.7

Waste reduction of expensive and complex medications can also extend into intravenous medication compounding, particularly in the oncology field where sustainability is vital8 as the global ‘load’ for IV-chemotherapy cancer treatments is estimated to increase from a 2018 baseline by 53% (from 9.8 million to 15 million individuals) by 2040.9
A gravimetric compounding solution such as BD Cato™ which can reduce the risk of compounding error (and the obligatory discarding of incorrectly compounded products) not only makes financial sense, it is also contributing to overall sustainability of oncology care. A well-constructed and extensive study in 2019 found the volume of potentially incorrectly compounded oncology products with a greater than 20% tolerance error for incorrect dose to be as high as 7.89% of all compounded products.10 When using BD Cato™ the clean room technician is also supported by the software to choose the most sustainable and economical option in terms of the menu of ampoule size selection for optimum dosing and the ability to optimally reuse partial ampoules of these high-value medications.

The compounding clean room is an engine room of productivity in IV-medication cancer care, and we need to think about the sustainability of technicians and pharmacists working in this area. Healthcare is a highly human industry, and it takes a heavy load on the people working within it. Technology can assist not only with reducing NVA, and potentially error loaded, tasks such as transcription from prescription to compounding order sheets, but also by supporting workflows with compounding with point of care guidance, key-step capture making review and second-check sign off easier and more effective, and through barcode label production that can track the compounded product’s journey right down to documentation of administration. A 2021 study illustrated how one oncology compounding unit increased its productivity over five years by 100% after the introduction of the BD Cato™ compounding solution without a change in employee headcount.11

Automating Community Services for Sustainability
When we look at the value given by the different services available in healthcare systems we need to think expansively and in terms of the econometrics of how we serve patients to maximize cost effectiveness, but also to ensure sustainability by making our cost analysis at a societal level. For example, community pharmacies and retail pharmacies have a potentially strong role to play in making healthcare sustainable by undertaking primary healthcare functions such as running weight reduction clinics, smoking cessation courses, diabetic care assessments and so on.

These retail and community pharmacies are potentially powerful agencies in maintaining the sustainability of healthcare systems. It is a logical extension to link them and integrate them into the processes of prescribing and medication management we already see in our large university and specialist hospitals and medical cities. Then, through applying automation in retail and community pharmacies to manage orders and inventory, we can free these professional pharmacists to take on extra services to serve patients better and more locally.
‘Localization’ through making smaller scale pharmacies as efficient as those already automated in large centrally located facilities works at another level of sustainability. Talking about the traffic for residents of our great cities in the Middle East is like talking about the weather for the English, and our cities are choked with automobiles. Connected and automated medication management for patients who are at home via community outlets and via ATM style medication dispensing units backed by BD Rowa™ medication storage and picking technology with telehealth support from pharmacists potentially reduces unnecessary car trips for medication refills to city central hospitals.

Over the last fourteen years, humanity has passed seven of eight safe boundaries for the Earth’s ecosystem to be able to support habitation12 and whilst air pollution remains just inside the threshold for ‘dangerous limits’ there are still 4.2 million deaths attributed to poor air quality globally per annum.12 Reducing traffic is very much a sustainability goal as it remains a substantial determinant of health in even developing economies.12 BD Cato™ technology has also been used to allow pharmacists to undertake accurate remote checks on compounding units, this garnered $23,770 in direct annual savings with no change in the quality of the checks in one study13, and we must consider that now unnecessary commutes could also be reduced by such an approach.
Sustaining the Environment, Sustaining the Healthcare Workforce
Healthcare also contributes to greenhouse gases in another way. A 2021 paper14 concluded that in our current climate crisis, sustainable healthcare initiatives need to look at the impact of inhaled anesthetics both on the wider environment and on the direct occupational environment of Health Care Workers (HCPs). This was essentially a call to action to judiciously consider in each treatment how, when, and why volatile agents such as nitrous oxide (N2O) and desflurane are unavoidable, and whether Total Intravenous Anesthesia (TIVA) and Target Controlled Infusion (TCI) of anesthetic agents via pharmacokinetic models of the types used in BD Alaris™ Plus PK syringe pumps could be efficacious substitutes, and to invest in the development of new technologies.
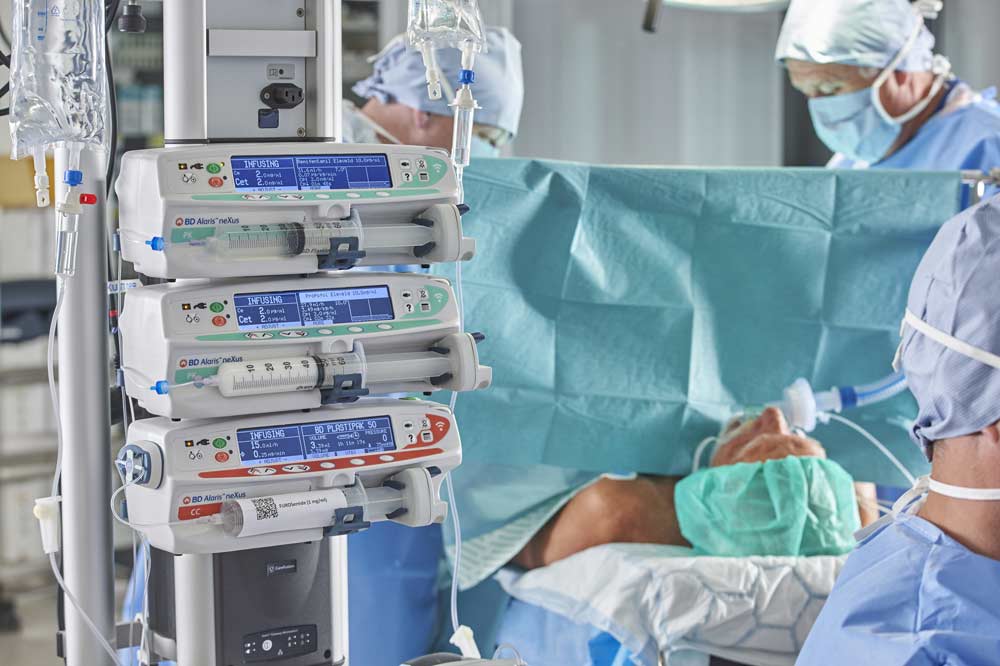
Sustainability also means looking after each other, and we need to work systemically to create and maintain a just culture, and to make sure that the systems within our facility ‘raise up’ and support all staff and increase the chance of them doing things correctly. System failures of risk management leave clinicians exposed, and at risk of burnout, and work overload, and increase the risk of patient harm.15 Sustaining HCPs, physicians, pharmacists, and nurses, is an area where we believe technology can contribute at many levels. Creating a feeling of confidence in the system in which HCPs work and reducing the risk of medication error can be achieved through the application of Dose Error Reduction Systems for intravenous therapy16 and with Automated Dispensing Cabinets with barcode scanning for patient identification and confirmation of ‘right medication’.17 The risk of attrition and ‘burnout’ in nurses must be attended to both urgently and continually if we are to maintain a sustainable nursing workforce.18
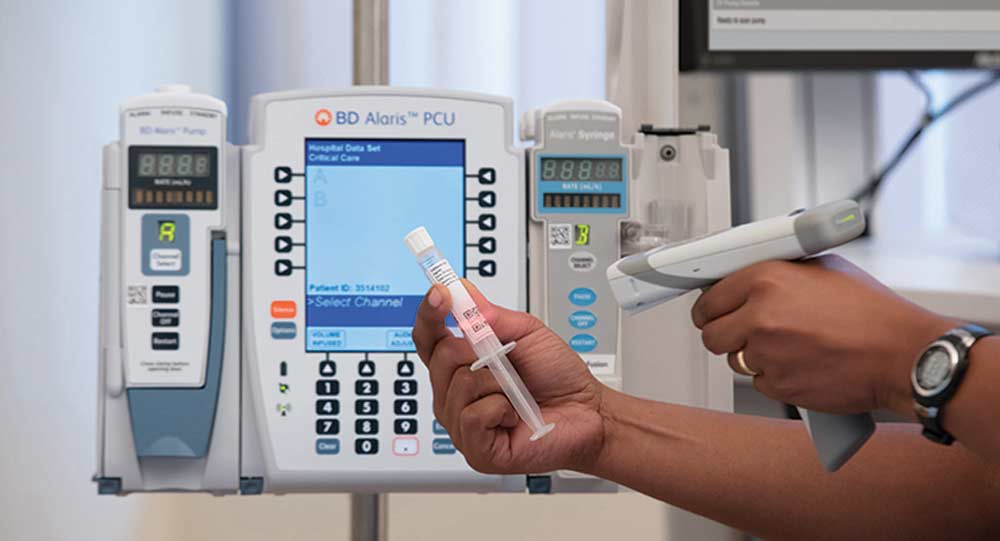
Medication error also impacts the financial sustainability of healthcare at a societal level. The OECD estimates that 15% of annual health spending globally is used for rectifying medical error, and of the adverse events causing this loss, 18.3% of them are medication errors.19 Serious medication errors can cost $7300 and 4.8 days in extra length of stay per episode.20
Sustaining Our Gains
Fleming’s discovery of Penicillin took place in 1929, so we have not sustained even one-century from this ‘game-changing moment’ before we witnessed the emergence of Antimicrobial Resistance (AMR). So how to ensure a future for this vital group of medications? The nightmare scenario has been with us for a number of years now, that the first, second, and third-line antibiotics fail against resistant organisms. Sustainable healthcare, and the ability to effectively treat patients in the future means using our skills and our technology to preserve our ammunition.
AMR control is therefore everyone’s responsibility. Reducing the risk of patients acquiring nosocomial complications or hospital-acquired infections leading to unnecessary extensions of stay, and extra lines of antibiotics is critical. All these adverse events take resources out of the available funding, and in the case of possibly avoidable treatment for nosocomial infections we have to take account of the ecological impact of IV-cannulation and disposables for IV-medications which add extra packaging and waste plastic to the environmental cost of reparative treatment.21
Reducing risk can range from ensuring optimal selection, insertion, and care of IV-catheters, through to IV-infusion strategies aimed to ensure longevity for peripheral and central venous access. There is also a strong economic and financial argument for adding quality to infusion therapies22 via specialist pressure monitoring techniques, filtration, and AI-predicted flow-rate manipulation to preserve venous access for as long as possible.23
Antibiotic stewardship is interdisciplinary- but it’s better done if we share, and if we have one common source of information that captures it all.24 Every patient’s journey is complex and BD solutions such as BD HealthSight™ Clinical and Infection Advisor that track antimicrobial usage and emergent infections in both the facility and in the community25 ensure that medication management and antibiotic stewardship data is available for collaboration and coordination of strategy between the infectious disease and microbiology departments and the pharmacy department to manage not only the patient but also the organization’s wider goals of antibiotic stewardship, antibiotic waste reduction, and efficiency in treatment.
BD solutions for medication management aim to take away non-value-added tasks and bring information to the right place at the right time to assist in sustaining patients and sustaining healthcare for all.
Not all products, services, claims or features of products may be available or valid in your local area. Please check with your local BD Representative. The information included in this article is intended for healthcare professionals only.
References:
1. https://www.bd.com/content/dam/bdcom-assets/en/en-us/documents/policies-guidelines-and-statements/policies/bd-global-expectations-for-suppliers_english.pdf
2. https://investors.bd.com/esg/sustainability
3. https://www.bd.com/en-us/about-bd/esg?#bd-tabs-f3430fd6ed-item-86472f67ba-tab
4. Al-Olah Y, Al Thiab K. Admissions through the emergency department due to drug-related problems. Ann Saudi Med 2008;28(6):426-429.
5. Fisher AM, Ding MQ, Hochheiser H, Douglas GP. Measuring time utilization of pharmacists in the Birmingham Free Clinic dispensary. BMC Health Services Research. 2016;16(1):529. doi:10.1186/s12913-016-1787-6
6. West LM, Diack L, Cordina M, et al Applying the Delphi technique to define ‘medication wastage’ European Journal of Hospital Pharmacy 2015;22:274-279.
7. Al Nemari M, Waterson J. The Introduction of Robotics to an Outpatient Dispensing and Medication Management Process in Saudi Arabia: Retrospective Review of a Pharmacy-led Multidisciplinary Six Sigma Performance Improvement Project. JMIR Hum Factors. 2022 Oct 11;9(4):e37905. doi: 10.2196/37905. PMID: 36222805; PMCID: PMC9597422.
8. Ferrara L, Otto M, Aapro M, Albreht T, Jonsson B, Oberst S, Oliver K, Pisani E, Presti P, Rubio IT, Terkola R, Tarricone R. How to improve efficiency in cancer care: Dimensions, methods, and areas of evaluation. J Cancer Policy. 2022 Dec;34:100355. doi: 10.1016/j.jcpo.2022.100355. Epub 2022 Aug 22. PMID: 36007873.
9. Wilson BE, Jacob S, Yap ML, Ferlay J, Bray F, Barton MB. Estimates of global chemotherapy demands and corresponding physician workforce requirements for 2018 and 2040: a population-based study. Lancet Oncol. 2019 Jun;20(6):769-780. doi: 10.1016/S1470-2045(19)30163-9. Epub 2019 May 8. Erratum in: Lancet Oncol. 2019 Jul;20(7):e346. PMID: 31078462.
10. Terkola R, Czejka M, Bérubé J. Evaluation of real-time data obtained from gravimetric preparation of antineoplastic agents shows medication errors with possible critical therapeutic impact: Results of a large-scale, multicentre, multinational, retrospective study. J Clin Pharm Ther. 2017 Aug;42(4):446-453. doi: 10.1111/jcpt.12529. Epub 2017 Apr 21. PMID: 28429389.
11. Meren ÜH, Waterson J. Evaluating An Automated Compounding Workflow Software for Safety and Efficiency: Implementation Study. JMIR Hum Factors. 2021 Nov 2;8(4):e29180. doi: 10.2196/29180. PMID: 34456182; PMCID: PMC8596227.
12. Rockström, J., Gupta, J., Qin, D. et al. Safe and just Earth system boundaries. Nature (2023). https://doi.org/10.1038/s41586-023-06083-8
13. Jean SJ, Francart SJ, Eckel SF, Schenkat D, Eberwein S, Lamm M, Barnes N, Valgus JM, Amerine LB. Evaluation of telepharmacy and the use of a gravimetric technology-assisted workflow system for remote sterile product pharmacist checks. Am J Health Syst Pharm. 2020 Mar 24;77(7):560 567. doi: 10.1093/ajhp/zxaa015. PMID: 32086506.
14. Gaya da Costa M, Kalmar AF, Struys MMRF. Inhaled Anaesthetics: Environmental Role, Occupational Risk, and Clinical Use. J Clin Med. 2021 Mar 22;10(6):1306. doi: 10.3390/jcm10061306. PMID: 33810063; PMCID: PMC8004846.
15. Van Gerven E, Vander Elst T, Vandenbroeck S, et al. Increased Risk of Burnout for Physicians and Nurses Involved in a Patient Safety Incident. Med Care. 2016;54(10):937-943. October 10, 2016.
16. Waterson J. Making smart pumps smarter, making IV therapy safer. Br J Nurs 2013 Jul;22(Sup13):22-27.
17 . Wang YC, Tsan CY, Chen MC. Implementation of an Automated Dispensing Cabinet System and Its Impact on Drug Administration: Longitudinal Study. JMIR Form Res. 2021 Sep
17;5(9):e24542.
18. Castro Lopes, S., Guerra-Arias, M., Buchan, J. et al. A rapid review of the rate of attrition from the health workforce. Hum Resour Health 15, 21 (2017). https://doi.org/10.1186/s12960-017 0195-2
19. Slawomirski L, Auraaen A, Klazinga N. Organisation for Economic Co-operation and Development: Paris, France; 2017. whttps://www.oecd.org/health/health-systems/The-economics-of-patient-safety-March-2017.pdf
20. Manrique-Rodríguez S, Sánchez-Galindo A, López-Herce J, Calleja-Hernández MÁ, Martínez-Martínez F, Iglesias-Peinado I, Carrillo-Álvarez A, Sanjurjo-Sáez M, Fernández-Llamazares C. Implementing Smart Pump technology in a pediatric intensive care unit: a cost-effective approach. Int J Med Inform. 2014 Feb;83(2):99-105.
21. Campion, Nicole & Thiel, Cassandra & Woods, Noe & Swanzy, Leah & Landis, Amy & Bilec, Melissa. (2015). Sustainable Healthcare and Environmental Life-Cycle Impacts of Disposable Supplies: A Focus on Disposable Custom Packs. Journal of Cleaner Production. 94. 10.1016/j.jclepro.2015.01.076.
22. Lim, S., Gangoli, G., Adams, E., Hyde, R., Broder, M. S., Chang, E., Reddy, S. R., Tarbox, M. H., Bentley, T., Ovington, L., & Danker, W. Increased clinical and economic burden associated with peripheral intravenous catheter-related complications: analysis of a US hospital discharge database. Inquiry: a journal of medical care organization, provision and financing. 2019:56, 46958019875562.
23. Kia A, Waterson J, Bargary N, Rolt S, Burke K, Robertson J, Garcia S, Benavoli A, Bergström D. Retrospective review of determinants of intravenous infusion longevity and infusion failure via a nonlinear model analysis of smart pump event logs. JMIR AI. Submitted May 2023. https://preprints.jmir.org/preprint/48628 (Pre-print, June 2023)
24. Zeana C, Palmieri FE, Gupta V, Ye G, Lao P, Yu K, Kang KS, Schiller L, Purswani M. Association between fluoroquinolone utilization rates and susceptibilities of gram-negative bacilli: Results from an 8-year intervention by an antibiotic stewardship program in an inner-city United States hospital. Sci Prog. 2021 Apr-Jun;104(2):368504211011876. doi: 10.1177/00368504211011876. PMID: 33908291.
25. Dunne MW, Aronin SI, Yu KC, Watts JA, Gupta V. A multicenter analysis of trends in resistance in urinary Enterobacterales isolates from ambulatory patients in the United States: 2011-2020. BMC Infect Dis. 2022 Feb 28;22(1):194. doi: 10.1186/s12879-022-07167-y. PMID: 35227203; PMCID: PMC8883240